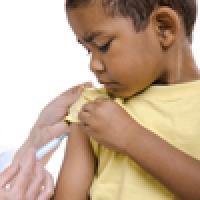
Who should be vaccinated first?
With all the questions in the news we asked experts Matt Keeling and Sam Moore, epidemiological modellers at Warwick University and members of the JUNIPER modelling consortium, who should be vaccinated first. Here is what we learned.
Since not everybody can be vaccinated at once, we need to decide who gets the vaccine first. There are two obvious strategies. One is to prioritise those with the most social contacts because they are most likely to spread the infection. This would probably involve vaccinating younger age groups first, as these tend to meet more people both through work and for fun. The other strategy is to prioritise the most vulnerable, so that's older people and people with specific health conditions that put them at higher risk.
Click here to see the entire COVID-19 vaccines FAQ.
Epidemiological modellers Matt Keeling and Sam Moore, together with Ed Hill, Louise Dyson, and Mike Tildesley, have explored the question of which strategy is better using mathematical models that can simulate how a disease will spread under specific assumptions (the models they used are sophisticated compartmental models, see this article to find out more).
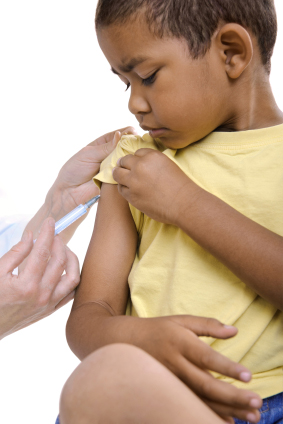
It makes sense to prioritise older people for the COVID-19 vaccine, so children will come later on in the queue.
When the team did their modelling over the summer and autumn it wasn't yet clear what type of vaccine was going to emerge and how effective it would be, so they explored a range of possibilities for the way a vaccine might work (e.g. does it suppress transmission or just symptoms?) and how effective it is (e.g. 50%, 70% or 90%). They also explored a range of different assumptions, for example about whether there are social distancing measures in place while the vaccination programme is happening, and whether the vaccine is deployed quickly or slowly (you can find out more about the scenarios that were explored and the underlying assumptions in the paper).
The outcome of the modelling is astonishingly clear: for all scenarios that were explored it appears better to prioritise the vulnerable — which corresponds to the elderly and those with underlying health conditions. This strategy will lead to a smaller number of deaths by the end of 2021, and it will also lead to a smaller number of QALYs lost — QALY stands for quality adjusted life year and is a measure of a period of a person's life that takes into account the quality of that life (see here to find out more).
This means that vaccinating people in the order of their age groups, starting with the over 80s, is the best strategy. People who are vulnerable because of underlying health conditions should also be vaccinated near the start of the vaccination programme. Health care workers are also prioritised due to their greater risk of coming into contact with the virus, the need to preserve our healthcare system, and the potential gains if the vaccine actually suppresses transmission. This is essentially the strategy the UK government has adopted, guided in part by the mathematical modelling.
If not enough people get vaccinated, and social distancing measures are not observed, then even the best vaccine can't win.
The modelling also suggests two other important lessons. The first is that, unless reasonably strict social distancing measures are in place, a race will ensue between an exponentially growing epidemic and a vaccination programme trying to keep up. This race may well be won by the epidemic — due to the speed of exponential growth. In fact, if all social distancing measures are lifted while vaccinations are underway, then the modelling suggests that only a very effective vaccine, which can suppress transmission as well as symptoms, will be able to control subsequent waves.
The second lesson is that the uptake of the vaccine is crucial. The modelling assumed that 70% of each subgroup of the population would be vaccinated. But if the uptake is significantly lower, then even the best vaccine can't win.
Return to our COVID-19 vaccines FAQ
About this article

Matt Keeling
Matt Keeling is a professor at the University of Warwick, and holds a joint position in Mathematics and Life Sciences. He is the current director of the Zeeman Institute for Systems Biology and Infectious Disease Epidemiology Research (SBIDER). He has been part of the SPI-M modelling group since 2009.
Sam Moore is a postdoctoral research associate who has been working on vaccination modelling for Covid-19 after joining SBIDER within the University of Warwick at the start of the pandemic earlier this year.

Sam Moore
Both are members of JUNIPER, the Joint UNIversity Pandemic and Epidemic Response modelling consortium. It comprises academics from seven UK universities who are using a range of mathematical and statistical techniques to address pressing question about the control of COVID. The universities are Cambridge, Warwick, Bristol, Exeter, Oxford, Manchester, and Lancaster. You can see more content produced with JUNIPER here.
Marianne Freiberger and Rachel Thomas are Editors of Plus.
