Can data science help rebuild our trauma networks?
Ambulance and A&E waiting times have been much in the news lately. It seems that many places could benefit from an increase in capacity, and here is where mathematics can help.
If we were to suffer a terrible injury here in Cambridge, the East of England Trauma Network would spring into action and an ambulance would take us to Addenbrooke's Hospital in Cambridge. But if we were elsewhere in the region, more than a 45 minute ambulance ride away from Addenbrooke's, we would be rushed to one of the twelve other hospitals in the region that complete the network.
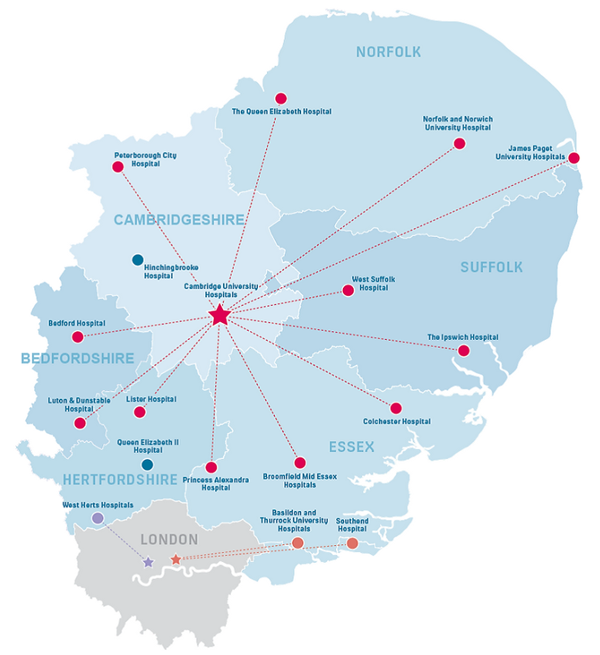
The East of England Trauma Network (Image used with permission)
Addenbrooke's is the only Major Trauma Centre in the region, meaning that it is the only hospital that can provide all the services that might be required. This means that patients initially cared for and assessed at other hospitals may have to transfer to Addenbrooke's to have further treatment if required. But a lot has changed over the ten years since the East of England Trauma Network was first established. "The number of beds for major trauma patients in Addenbrooke's is the same, but the number of patients has increased," says Houyuan Jiang, Professor of Management Science at the Judge Business School. "Demand is increasing because the size of the population is getting bigger and the population is getting older. It's time to reassess the service needs and supply."
Improving a trauma network
Jiang, along with colleague Feryal Erhun, Professor of Operations and Technology Management at the Judge Business School, are members of the Cambridge Mathematics of Information in Healthcare Hub (CMIH), a collaboration of 19 co-investigators from different disciplines across the University of Cambridge who use mathematics to meet the data challenges across all types of medical treatments. (You can read more about CMIH here.) Jiang was speaking at a CMIH event in June 2023, organised by the Newton Gateway to Mathematics, about his work supporting the development of the East of England Trauma Network to meet the future healthcare needs of the people in the region.
The proposal is to build a second Major Trauma Centre by upgrading the Trauma Unit at one of the other hospitals in the region. But where should it be? How many beds for major trauma patients should it have? And will this meet the demand across the network? Like many of the researchers in CMIH, Jiang used a machine learning approach to draw on the extensive amount of data available to derive possible answers to these questions. (You can read an easy introduction to machine learning here.) Jiang and his colleagues used data from the past ten years relating to the use of the trauma hospitals in the region, as well as projections (from the Office for National Statistics) for how the population will change into the future and the impact this would have on demand. They also drew on information from Google Maps to judge distances of potential patients to hospitals.
Once Jiang and his colleagues had built machine learning models based on these extensive data sets, they used counterfactual analysis to explore how much you have to change the inputs into the models (say, the location of the Major Trauma Centre, or the number of major trauma beds) to affect the output of the model (say, that the network can meet demands in the required amount of time). Machine learning models can often appear to be mysterious black boxes and counterfactual analysis can help researchers explain and interpret what their models are doing.
Bringing the CMIH family together
Jiang's work on using a mathematical data driven approach to infrastructure and planning decisions in health care was just one example of the wide range of work done by members of CMIH at the event. Also speaking was neurosurgeon Chao Li, who explained how image analysis algorithms can help with the diagnosis and treatment of brain tumours. And biomedical physicist Sarah Bohndiek discussed some of the promising medical applications of using multispectral imaging, where objects are imaged using many different wavelengths of light. One potential application would be new medical equipment that could help spot, and so treat, precancerous regions in the oesophagus, stopping them developing into cancer.
A beautiful example of multispectral imaging
The breadth of speakers at this event and the links between their work really demonstrated the range and strength of the multidisciplinary collaboration supported by CMIH. "The CMIH is quite diverse in terms of research topics, with early career researchers, and with people coming from different disciplines and from industry," says Carola-Bibiane Schönlieb, Professor of Applied Mathematics at the University of Cambridge and Co-Director of CMIH. "We all have in common a passion for bringing data analytics into clinical research."
James Rudd, Professor of Cardiovascular Medicine and Clinical lead of CMIH, said the work produced by the CMIH had already resulted in real impacts on the healthcare received by patients: "Quite a few [of the nearly 100 papers produced by CMIH so far] have impacted policy. For example, a model [developed by CMIH] for waiting lists for cardiovascular disease is now being used by NHS England."
And although the event marks the end of this phase of the CMIH, Schönlieb says that there are major developments in healthcare analytics that this group of researchers can play an important role in. One area of potential future work, which she suggested could become CMIH3, is looking at interfacing the mathematics and data science behind the health of our population, with that behind the health of our environment. Looking at these two societal challenges in a unified way may be the next frontier.
About this article
This article is based on a talk by Houyuan Jiang at the CMIH Academic Engagement Event which took place on 21 June 2023, hosted by the Newton Gateway to Mathematics.
The work Jiang spoke about is led by Dr Esther Kwong, Specialised Commissioning Public Health Consultant from the Healthcare team at NHS England. The collaboration with the Judge Business School at the University of Cambridge was established for capacity modelling and forecasting. Esther Kwong, Lauren Rixen, Zidong Liu, Feryal Erhun, and Houyuan Jiang have authored a report on this work, Public Health Needs Assessment for Major Trauma, which will be publicly available later in the year.
Rachel Thomas is Editor of Plus.
This article was produced as part of our collaborations with the Cambridge Mathematics of Information in Healthcare Hub (CMIH), the Newton Gateway to Mathematics and the Isaac Newton Institute for Mathematical Sciences (INI).
The INI is an international research centre in Cambridge which attracts leading mathematicians from all over the world. The Newton Gateway is the impact initiative of the INI, which engages with users of mathematics. You can find all the content from the collaboration here.

